|
Presentation
|
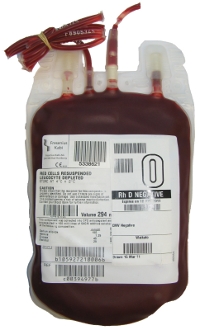
- Resuspended Red Cells - 220-340mL
- Paediatric Packs - each donation is divided into 4 paediatric
doses - 55-85mL
- Haematocrit-adjusted blood is used for neonatal exchange transfusions and intrauterine transfusion
- Whole Blood - 405-513mL
 |
|
|
ABO & RhD Compatibility
|
ABO
- a group O patient can receive only group O red cells
- a group A patient can receive group A or O red cells
- a group B patient can receive group B or O red cells
- a group AB patient can receive group AB, A, B or O red cells
- ABO incompatible transfusions can be fatal. Always check the the red cells against the patient at the bedside.
Rh(D)
- Transfusion of red cells are normally Rh(D) identical
- Rh(D) negative red cells may be given to Rh(D) positive
recipients without creating any risk for immunisation
- In life threatening emergencies, Rh(D) positive cells may be
given to an Rh(D) negative recipient but there is a risk that
this will stimulate the production of anti-D. The Blood Bank will
provide guidance. The Clinician must be notified.
- Rh(D) positive red cells may be provided by the Blood Bank
for males, and for females beyond reproductive years, if supplies
of Rh(D) negative red cells are low.
|
|
Storage
|
- Must be stored in an appropriately monitored (2-6°C) blood refrigerator
according to Blood Bank standards. Never store in a drug or food fridge.
- If the transfusion can not be started within 30 minutes,
return the component to the Blood Bank immediately for
appropriate storage.
|
|
Filter
|
- Use a standard blood infusion set that has a 170-200 micron
filter.
- ANZSBT guidelines require that blood giving sets must be changed when transfusion is completed or every 12 hours if the transfusion episode is not yet complete. This is intended to reduce the risk of bacterial growth occurring.
- Any number of red cell units may be transfused during a 12-hour period provided the flow rate remains adequate. However specific manufacturer's recommendations defining the maximum number of units per blood administration set must not be exceeded.
- A new blood administration set should be used if infusion of another fluid, medication or platelets is to continue after the current transfusion. This is intended to reduce the risk of incompatible fluids or drugs causing haemolysis of residual red cells in the administration set or drip chamber.
- Please consult your DHB blood policy for further details.
- All fresh components, including FFP and cryoprecipitate, are leucodepleted
at source by NZBS. No bedside leucodepletion is necessary.
|
|
Pump
|
- If necessary, approved infusion pump devices may be used.
|
|
Rate and Duration
|
- Paediatrics:
- top-up transfusion in a non-bleeding patient is typically given at 5mL/kg/hr
- exchange transfusion: depends on stability of the baby - discuss with NICU consultant
- resuscitation: rapid infusion based on the patient's haemodynamics
- Adults:
- top-up transfusion in a non-bleeding patient: most adults will tolerate one unit every 90 minutes. Consider a slower rate in patients with or at risk of congestive cardiac failure
- resuscitation: rapid infusion based on the patient's haemodynamics
- Infusion of all components should be completed within 4 hours of leaving refrigerated storage.
|
Monitoring | |
|
DO NOT
|
- DO NOT add medication to red cell components
- DO NOT use 5% Dextrose solutions (may induce
haemolysis)
- DO NOT use Lactated Ringer's or other balanced salt solutions that contain Calcium, as this may
induce clot formation in the blood bag and / or administration set.
|
|
Dose
|
- 4-5mL/kg will raise the patient's Haemoglobin level by approximately 10g/L.
- It is recommended that the patient's haemoglobin be checked between units if giving multiple units.
- For paediatric patients, the dose should be written in mL, not units.
|
|
Dose calculator
|
|
|
More Info
|
|
|
